Tonsillectomy and Adenoidectomy in Children
What are Tonsils and Adenoids?
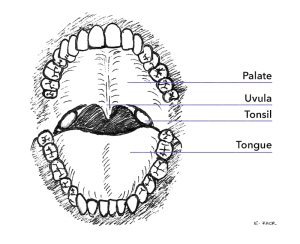
Tonsils and adenoids are collections of lymphoid tissue in the oral cavity and postnatal space respectively. There is a tonsil on each side at the back of the mouth, they are usually visible with the uvula hanging down between them. The adenoid is located in the back of the nose and as such it is not normally visible through the mouth.
Being lymphoid tissue they play a role in immune function. There is however a large amount of other lymphoid tissue in the head and neck so the immune system does not rely entirely on the tonsils and adenoids. Studies have not shown an increase in upper respiratory infections if the tonsils and adenoids have been removed.
Indications for Surgery - Adenotonsillectomy
The operation
Adenotonsillectomy is performed in hospital under general anaesthesia. I do not perform Adenotonsillectomy as a day procedure in children. All patients will be in hospital overnight after surgery. Children under four are normally admitted to the high dependency area for closer observation of the airway and oxygen levels, particularly children with a history of sleep apnoea. A parent is welcome to stay with the child overnight.
There are many ways to remove the tonsils and adenoids; these include gentle dissection, coblation, bizact, laser, partial tonsillectomy and the use of a microdebrider.
In the past I have had experience of all these methods. I have found that the safest method with the lowest complication rate and least pain is using the Bizact device to remove the tonsils. This device cauterises vessels and cuts with very little if any blood loss and minimises trauma to the tonsil bed.
After surgery
The first night
All children will be kept in hospital overnight. They will have intravenous access for fluids and anti-nausea and vomiting medication. Most will be able to have dinner but some children will not feel like it.
Discharge from hospital
The majority of children will be ready for discharge mid morning the day after surgery. Before they go home however they must be tolerating a normal diet and consuming adequate fluids. I don't sent children home until they are ready.
Diet
A normal diet post operatively is important as the passage of food keeps the tonsil beds clean. A soft diet such as soups and ice-cream does not do this as effectively as meat, bread and vegetables.
Activity
For 10 days post operatively the child needs to be kept calm and quiet in the care of a responsible carer. During this time they should not go to school and avoid excessive activity such as parties, playgrounds etc.
Pain relief
Most children tolerate the surgery very well. That said there is some pain which is usually managed adequately with paracetamol. For the first few days it is best to give paracetamol regularly but take care not to exceed the maximum daily dose. Don't be surprised if the pain improves and then worsens again around a week after surgery as this is the time of peak inflammation. It is also not unusual to have earache which is referred from the tonsil bed.
Codeine containing pain relief medication must not be used with out first discussing with Dr. Varley as it can be dangerous in children.
Nurofen likewise should not be used.
Appearance of the tonsil beds
After the tonsils have been removed the pockets they sit in are left open. They become covered with a layer of yellow/white slough. This is a normal appearance and does not indicate infection. The breath is normally a little smelly.
Bleeding
Bleeding after tonsillectomy occurs in around 1% of cases. It most commonly occurs the first night whilst in hospital or at around a week post operatively. Bleeds on the first night usually need to go back to theatre. Delayed bleeds are usually minor and don't need to be returned to theatre but the child will need re-admission to hospital for observation.
It is important you contact Dr. Varley if you notice any significant bleeding.
Postoperative instructions
You will be given instructions for care upon discharge. These are also available to download here. At discharge you will also be given a post-operative appointment and my mobile phone number.